proceedings of the tenth annual meeting of the American Academy of
Pediatrics) Journal of Pediatrics 18:538-547.
DeMarsh QB, Alt HL, Windle WF, Hillis DS (1941) The effect of depriving the
infant of its placental blood; on the blood picture during the first week of life.
JAMA 116:2568-2573
Wilson EE, Windle WF, Alt HL (1941) Deprivation of placental blood as a
cause of iron deficiency in infants. Am J Dis Child 62:320-327.
DeMarsh QB, Windle WF, Alt HL (1942) Blood volume of newborn infant in
relation to early and late clamping of umbilical cord. Am J Dis Child
63:1123-1129.
Vaughan K (1944) Why tie the cord? [letter] British Medical Journal (Jul 8):58
Chesterman CC (1944) Why tie the cord? [letter] British Medical Journal (Jul
22):125
Jackson GA (1944) Why tie the cord? [letter] British Medical Journal (Jul
22):125
Medical Journal 1947,Apr;50 (7):726-728.
the newborn; studies on sinus blood on the first an third days. American Journal
of Diseases of Children 75:860-871
placental blood and its effect upon the newborn; part I. California Medicine
71(3):190-196.
infants: a theory as to its cause and a method of prevention. Journal of
Pediatrics 36:421-426.
transfusion. N Engl J Med. 1954 Apr 15;250(15):629-32.
warhrend der Nachgeburtsperiode. Zentralblatt fur Gynakologie 76(9):329-341.
cord; its influence on the blood volume of the newborn. Obstetrics and
Gynecology 10:603-610.
respiratory distress syndrome. Pediatrics 24:1069-1100.
newborn. British Medical Journal (Jan 17):134-138.
Leak WN (1959) When to tie the cord [letter]. British Medical Journal (Feb 28):
584.
hypertension in the newborn infant associated with delayed clamping of the
umbilical cord Acta Paediatrica 50:149-159
1962 (Jun 9):1222-1223.
p894 - "It became necessary to include private patients in the premature group
to increase enrollment; the planned randomization of these infants as to time of
cord clamping failed." -- What an outrageous statement. Consent was
apparently not given by private patients to be randomly assigned to one group
or another. Only clinic patients, those without means to pay for private care -
childbirth was not covered by medical insurance in 1963.
28;1(7483):201-2
remarked:
clamping. Every physician employs a different technic and usually
establishes a pattern that he carries out routinely in his obstetric
work. At times this pattern is influenced by the equipment, the
nursing situation, hospital policy in care of the newborn and various
emergencies arising in the mother or the infant...
"It has been observed that the cord is often clamped immediately,
either as a routine procedure or so that the infant can be handed to
nurse for resuscitation and aspiration."
placental transfusion, that they would strip the cord three or four times to
squeeze all residual blood into the child. A survey in 1950 of 1900 members
of the American Board of Obstetrics and Gynecology found two thirds
regarded placental transfusion as a matter of minor importance, but nearly
one quarter (455) used the stripping procedure (McCausland et al. 1950).
In the same year, Landau et al. (1950) determined that immediate clamping of
the cord after Cesarean section was leaving the newborn in a state of
hypovolemic shock, which they were able to counteract by holding the
placenta above the infant to obtain drainage through the still intact umbilical
cord.
immediate cord clamping, delayed cord clamping with infant above or below
the level of the uterus during the period of postnatal transfusion, and
stripping. In the group subjected to immediate clamping, some of the red-cell
and hemoglobin levels were thought to be alarmingly low. Postnatal
transfusion with the infant held above the level of the uterus appeared
comparable to that with the infant below the uterus, the reason apparently
due to uterine contractions - though the infant heart may have a lot to do with
regulating blood flow back to the placenta. Stripping the cord led to the
highest red-cell and hemoglobin values.
Although stripping the cord is not totally natural, Colozzi's concluding
comments are worth keeping in mind:
episode, the physician is in great hast to clamp the cord and give a
pale, listless infant to a nurse for aspiration and resuscitation.
Usually, these infants are described as having asphyxia pallida, and
their prognisis is grave. They respond poorly to oxygen
administration, and worse to other heroic measures of resuscitation.
Their main difficulty is shock and blood loss, which are inadeqately
corrected by oxygen and are not improved by rough handling. I
have see several infants with asphyxia pallida who were very pale
and listless, with a rapid pulse and a very weak cry; with gentile,
slow, methodical cord stripping, they were transformed within a few
minutes to ruddy, lustily-crying infants."
delivery, which is said to occur in 25 to 30 percent of cases:
two of cord around its neck. Usually, the most expeditious measure
is to clamp and cut the cord in situ. This actually amounts to
immediate clamping in an already depressed baby. Every effort
within reason should be made to slip the loops over the infant's
head and allow it the benefit of its own blood."
controlled trials." These continue to the present day, for what reason it is had
to fathom. If only heed were paid to the non-invasive research data that
awaits rediscovery in medical journals going back over 130 years ago. Even
then, research was carried out assigning groups of infants to early and some
to delayed cord clamping. The major difference from such research today is
the difference in what was considered early or delayed.
1879), Ribemont (1879 -1881), vonEngel (1885), Kostlin (1898), Haselhorst
(1929) and Allmeling (1930) measured weight-gain in newborn infants during
the period of continuing umbilical cord pulsation. They collected data on 100
babies. They found that during the first minute after birth infants received on
average 78 percent of the total transfusion, with loss and gain fluctuations in
the succeeding minutes, diminishing up to 12 minutes after birth.
infants. In the first group, born between January 1957 through May 1959, the
cord was ligated immediately after birth except in cases in which mucus first
had to be aspirated from the pharynx; good judgement based on instinct was
thus revealed. The second group of infants, born between June 1959
through June 1961, the cord was clamped three to five minutes after delivery.
The number of cases of pulmonary syndrome was significantly less in the
second period, and the reduction was most significant in low birth-weight
infants (1501-2000 g).
Bound et al attributed the improved outcome to the delayed ligation of the
cord in the second group, concluding that, "Receipt of an adequate amount
of placental blood is an important factor in the prevention of the pulmonary
syndrome in premature babies." They suggested that delayed ligation of the
cord should become a standard procedure at the delivery of all premature
babies.
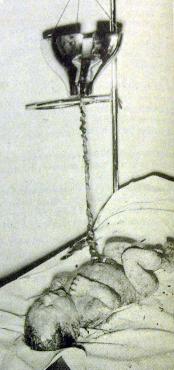
for providing postnatal placental transfusion
to infants born by emergency Cesarean
section, by removing the placenta with the
baby without cutting the cord, and placing the
placenta in a funnel hung above the baby
(see picture to right). For comparison, they
did the same with vaginally delivered babies,
using a temporary clamp on the cord until the
placenta was delivered.
Secher and Karlberg cited several earlier
investigations of placental transfusion
volumes (Haselhorst 1929, Allmeling 1930,
deMarsh et al. 1942, Ballentine 1949, and
Hormann & Lemits 1954). They noted, "Late
clamping of the cord has been an accepted
rule in normal deliveries, and its importance
was pointed out by Erasmus Darwin as early
as 1801." The Cochrane Review should have
included all of these earlier studies on the
benefits of placental transfusion.
sprepu